


To make an appointment call
305-448-4433

The Root Canal Specialists
Thank you for visiting Gables RCT Endodontics. Here you can find information about the services we can offer you. We know that visits to the dentist are stressful and our team is committed to providing you with a professional, warm and humane service to make your appointment as pleasant as possible.

Our Mission
Our first and foremost goal is to provide unsurpassed clinical excellence in a compassionate environment and have EVERY SINGLE PATIENT leaving our office satisfied.
Because we value highly the input of your dentist when determining the best treatment options for our patients, we keep in continuous communication with your dentist to verify that your needs are addressed in a comprehensive manner. We are attentive to your concerns and take great care to explain in detail the problem and the treatment options. We do all these in a manner you can easily comprehend thereby enabling you to make an informed decision with realistic expectations of the results. We attend patients promptly and will gladly fit endodontic emergencies into our schedule.
We look forward to serving you and we encourage you to call or visit our office to discuss any issues relating to our specialty.
Services
Root Canal Therapy or Treatment
A Root Canal is a common procedure performed to save a tooth where the pulp tissue is no longer healthy. First a local anesthetic, the same anesthetic a dentist uses for a filling is used to block all sensations from the tooth. The tooth is isolated using a rubber-dam to prevent potentially infected saliva from entering the canal system. Access is made into the pulp chamber, the canals, are located, most of the time with the help of an operating microscope. The canals are cleaned, shaped and disinfected. The tooth is dried and the canal spaces are sealed. At the completion, the tooth is restored either with a permanent restoration or a temporary one following your dentists instructions.
Re-treatment or second Root Canal Treatment
With proper endodontic treatment most endodontically treated teeth will function as long as your natural teeth. In certain cases, either teeth fail to heal after the initial treatment or the pain returns even years after the initial Root Canal Treatment was performed. If the structure of the tooth is not compromised, in most cases a second root canal treatment can restore the health and function of your tooth.
Endodontic Microsurgery (apicoectomy)
It is the use of an operating microscope and micro instruments to treat an infected root using a surgical approach. Surgical instrumentation is sometimes necessary if a tooth fails to heal after a conventional Root Canal Therapy.
Our Specialists

Ernesto Paz D.M.D.
Graduated Valedictorian of his class from Nova Southeastern University School of Dentistry in 2002. He then completed the post graduate program in Endodontics at Nova Southeastern University in 2004 and has been practicing the specialty of Endodontics at Gables RCT since then. Among his achievements: * Award of Excellence in 2001 from Omicron, Kappa, Upsilon Honor Dental Society. * Dean’s Award for highest ranking student in the class of 2002. * Research Published in the Journal of Endodontics in 2005. * Active Member of the AAE, ADA, and various local study clubs.



Eileen Lujan D.M.D.
Graduated from the University of Florida, College of Dentistry in 1995. She completed a General Practice Residency Program in 1996 at Mt. Sinai Medical Center followed by a post graduate specialty program in Endodontics at New York University College of Dentistry which she completed in 1999. Dr. Lujan joined Gables RCT in 1999 and has been practicing the specialty of Endodontics since then. She also served as President of ADCH and SDDS and has given several lectures to various local dental societies.
Technological advances in Endodontics
The continue research in the field of endodontics has led to the development of new equipments and therapeutic techniques:
Endodontist
An endodontist is dentist with two or more years of advanced training in the scope of Endodontic who has received a certificate in Endodontics from an advanced education program accredited by the ADA Commission on Dental Accreditation and who limits his or her practice to Endodontics.
Endodontics
Endodontics is a specialty of odontology oriented to the prevention, diagnosis and treatment of the pathological conditions of the dental pulp and its supporting structures.
Dental Pulp
The pulp tissue is compose of blood vessels, nerves, specialized cells and connective tissues and it is responsible for the formation of the root dentin and serves to perceive external stimuli.
Rotary Instrumentation
They are flexible instruments adapted to rotating equipment that allow a more predictable cleaning and shaping of the canals.
Electronic Apex Locator
It allows us to have greater accuracy when determining the length of the canals and also reduce the number of radiographs needed during length measurements.
Ultrasonic Instrument
It is used to remove obstructions like calcifications to gain access to the radicular canals. The acoustic streaming debrides the canal surfaces and gives us the ability to clean and disinfect irregular canals and it is also used to clean and shape the canal during periapical surgeries.
Microscopes
The use of magnification in Endodontics has been of vital importance. It improves visibility making it possible to find canals otherwise invisible to the naked eye.
Digital Radiography
Radiographs are taken with a digital x-ray sensor and the images are almost immediately available for viewing on a computer screen. Allowing speed, efficiency and decreasing the exposure of radiation to the patient.
Cone Beam Computed Tomography (CBCT)
A CBCT (cone beam computed tomography CT scan), helps dentists diagnose and treat patients. It involves the CT scan rotating around the patient’s mouth, taking pictures in the process to create the 3D x ray images. The American Association of Endodontist considers CBCT the preferred imaging modality for endodontic treatment in many clinical situations.
With the addition of a new CBCT machine, we are now able to offer our patients the latest technology in 3D imaging to improve the diagnosis and treatment of many cases.
Root Canal Treatment Step by Step
Root Canal Retreatment Explained
Cone Beam Computed Tomography
Gallery

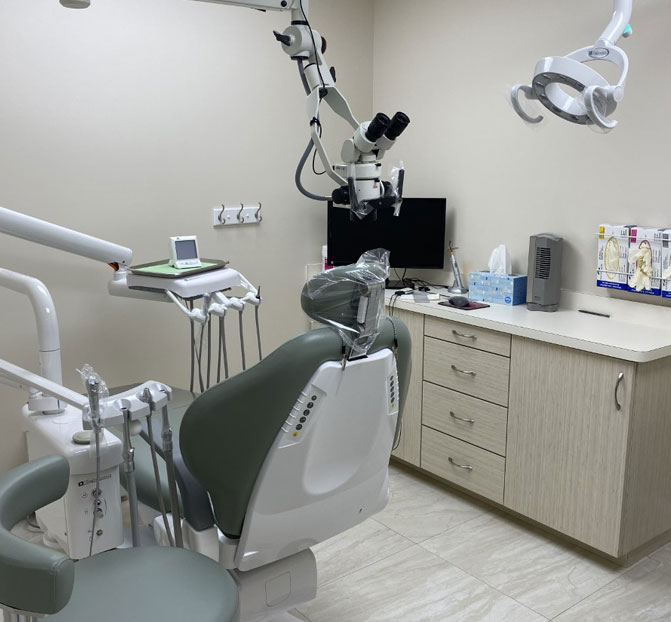
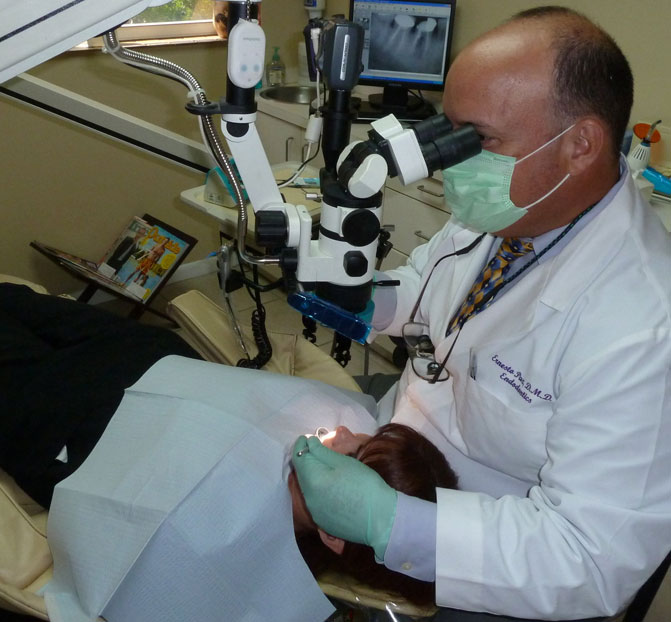

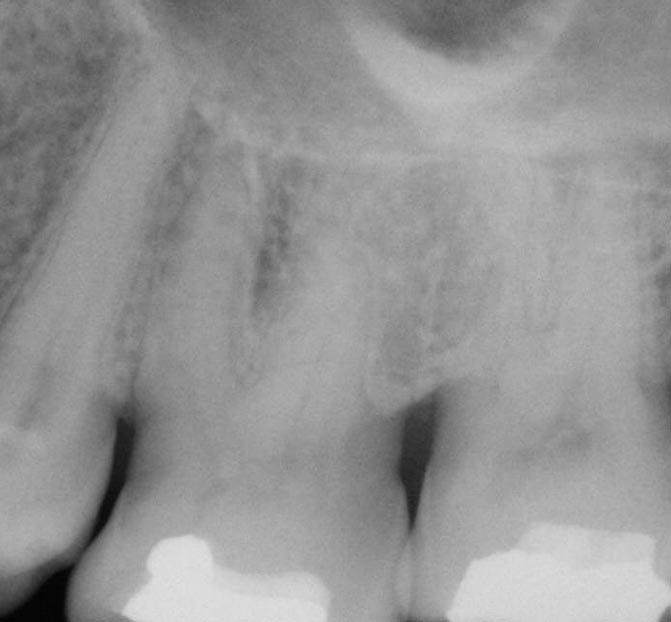

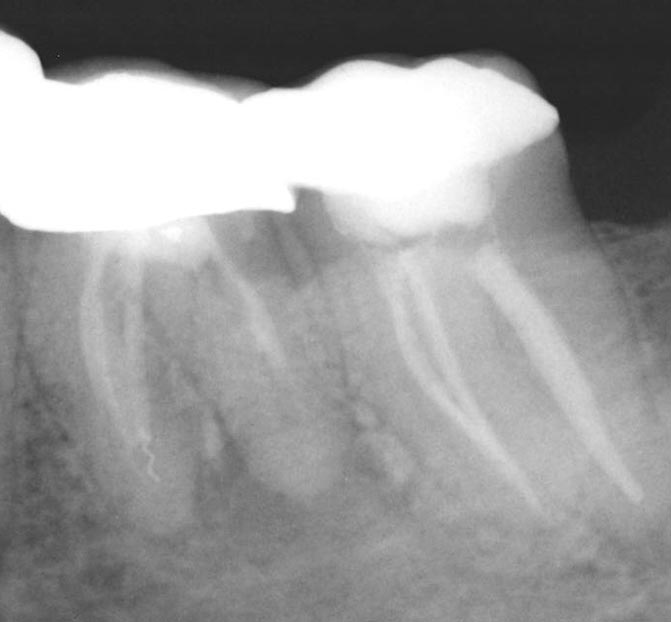
Frequent Questions
Most Root Canals are performed because of infection or inflammation of the pulp tissue (pulpitis) caused by caries, dental trauma or fractures. Inflammation of the pulp tissue (pulpitis) is accompanied by severe sensitivity or pain to thermal changes (hot or cold) that tends to linger. Not treated, it will result in death of the pulp tissue (necrosis) with disappearance of the symptoms to temperature. A necrotic pulp leads to infection of the supporting tissues of the tooth with pain to biting and later this could develop into an abscess with severe pain and swelling. If endodontic treatment is not performed, this infection and bone destruction could lead to the loss of the tooth.
Some of the signs include pain, swelling or significant sensitivity to hot or cold, discomfort to palpation and to biting. However in some cases radiographic findings with no history of symptoms could alert your dentist of the possible need for Root Canal Therapy.
Immediately after the treatment the area will still be anesthetized and that feeling could last 2 to 3 hours after leaving the office. Once the anesthetic wears off you could feel mild to moderate discomfort that in most cases can be controlled with over-the-counter analgesics.
After Root Canal Therapy the tooth will be sensitive to the bite and this sensation usually lasts a few days. However some cases do require longer healing times. We strongly recommend not biting on the treated tooth until the permanent restoration is placed to avoid fractures to the remaining tooth structure. In most cases the permanent restoration could be started 2 weeks after the Root Canal Therapy is completed.
Most teeth can be treated with Root Canal Therapy with a high rate of success. In cases where the canals can not be negotiated, the structure of the tooth is not enough to support a permanent restoration, the surrounding bone is not adequate or the roots have significant fractures the tooth will require extraction.
It is the use of an operating microscope and micro instrument to treat an infected root using a surgical approach. Surgical instrumentation is sometimes necessary if a tooth fails to heal after conventional Root Canal Therapy.
The tissue covering the infected root is elevated exposing the bone defect caused by the infection. The area is cleaned and the tip of the root is removed. In most cases the end of the canal is cleaned and shaped using specialized micro instruments. The canal is then sealed and the tissue is sutured in place.
Mild to moderate discomfort with localized swelling and bruising in the area of the surgery is to be expected. Antibiotics are usually not necessary after the surgery. However, pain medication will be needed for the first few days following the surgery. You will need to return to our office in 5 to 7 days for evaluation and suture removal. In office post operative instructions will be provided the day of the surgery and you are urged to contact our office if any concerns develop after your surgery .
The Root Canal retreatment is usually more elaborate because all previous root canal sealing materials will need to be removed to clean the canal system of the tooth. During the Re-treatment the canals will need to be re-cleaned and this usually requires gaining access to the inside of the tooth by making a small opening through an existing crown or cutting off the crown altogether. The recovery of a retreatment is similar to the recovery of an initial root canal therapy. In most cases, mild to moderate discomfort will last only a few days. As with a standard Root Canal Therapy, the re-treated tooth should have a permanent restoration as soon as possible. We recommend that you make an appointment with your dentist 1 or 2 weeks after the Endodontic Treatment is completed so that your dentist can restore your tooth back to function.
Contact Us
45 SW 36 CT
Miami, Florida 33135
Phone: (305) 448-4433
Fax: 305- 441-2821
Email: gablesrct@gmail.com
